Part 3: The Science of Surfaces Series
Part 3: How do Pressure Ulcers Form?
Shear and Friction
In part 2, we looked at the effect of pressure on the skin. In this instalment, we will now look at shear and friction.
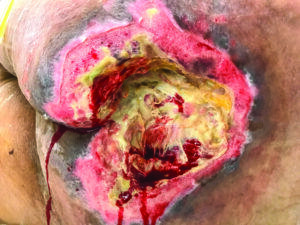
Shear can occlude blood flow and can be very significant in the cause of pressure ulcers1. In a hospital environment, shear strain can occur when an individual slides down the bed, and the skin remains stationary but there is a difference in movement of the underlying soft tissue such as the muscles2. This vigorous inter-tissue movement causes stretching and tearing of blood vessels, reducing blood flow leading to ischaemic tissue necrosis (death of most or all cells)2.
Friction is defined as the rubbing of one entity against another or a force that resists motion between two bodies in contact and/or material elements sliding against one another3. Friction can contribute to the formation of pressure ulcers indirectly; friction is necessary to create the shearing forces1. Skin will be weakened by pressure and will most likely be more susceptible to the motion of friction and with these two risk factors working together it will accelerate the breakdown of skin1.
Friction alone is not a direct cause of pressure ulcers but may exacerbate or contribute to the development due to the shear strain it can cause3. When considering the effects of shear and friction, the bed frame is an element to think about as research conducted by Rush (2018)4 identified that bed design had a substantial effect on migration down the bed and with the occurrence of migration there was increase in pressure. The research demonstrated that if a bed frame does not fully extend to fully accommodate the lengthening of the spine, it will cause a patient to slide down the bed4.
A bed frame with an elliptical backrest that can support the natural extension of a patient’s spine will create zero migration reducing the risk of shear and friction4. Read more about the elliptical backrest and the evidenced zero migration on the Medstrom Solo hospital bed frame here.
Click here for Part 4 of this series where we look at the effects of moisture on pressure ulcer formation.
To view the other pages in this series, click on the links below:
The Science of Surfaces Series
Part 1: How do pressure ulcers form?