Part 1: How Can I Prevent Complications From Immobility? Cardiovascular
Part 1
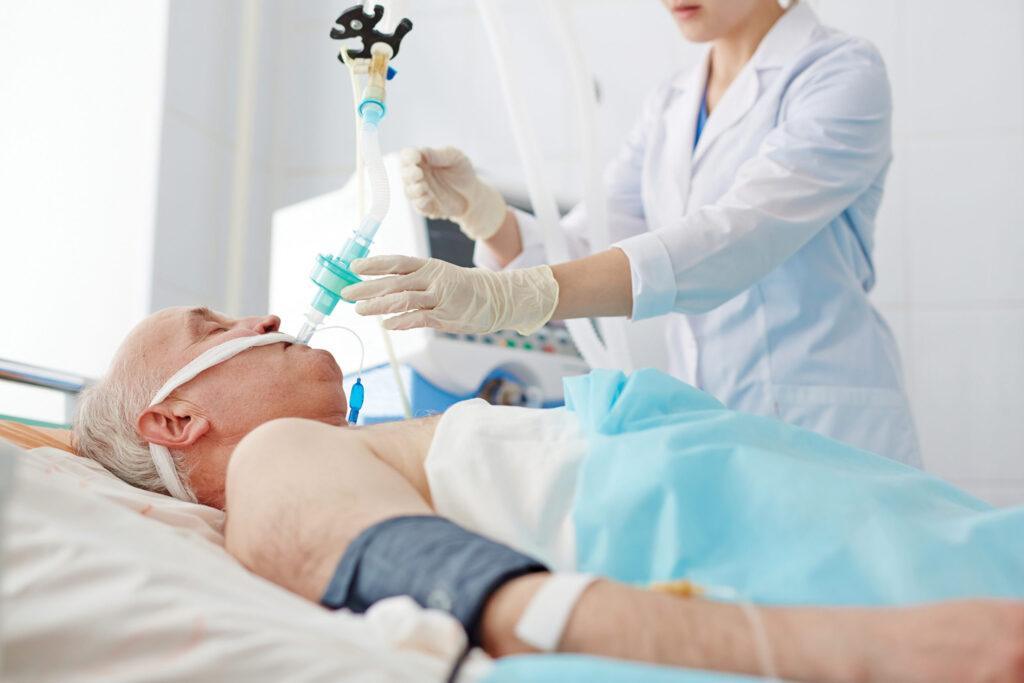
Nurses apply their knowledge daily to the consequences and complications of various health related diseases and disorders. Immobility has a great impact on not only the patient, but the healthcare professional. As basic principles of nursing care are applied to the care of the patient, the nurse is also aware of the many complications that may occur as well as the risk factors, signs, and symptoms to prevent these complications. Some injuries and illnesses (example, critical care) require that a person remains in bed and immobile for long periods. Not only can this be emotionally difficult for a person, especially one who is typically very active, it can also have adverse effect on their body.
Each body system is affected differently by a long period of immobility, as the body becomes more immobile the various body systems including Cardiovascular, Respiratory, Haematological, Gastrointestinal, Renal and Musculoskeletal can undergo dramatic changes and sometimes these changes can cause irreversible damage to the patient. The first body system we will look at is Cardiovascular.
Cardiovascular
It may be surprising; however, three weeks of complete bed rest can result in cardiovascular decline similar to that of 40 years of aging1. Immobilisation leads to structural changes in the cardiovascular system, including the reduction of venous return, increased heart rate and deconditioning which in turn affect its functionality.
Water loss and cardiac reconditioning are the most pronounced symptom of these changes, creating a tendency toward fainting when moving from lying to standing. When a patient has been in the supine position for a length of time, up to 1 litre of fluid can move from lower limbs to the chest area. In the short term, this raises venous return and increases intracardial pressure. Therefore, the monitoring of fluid intake and urine output is vital when the patient is immobile. When the patient attempts to regain mobility, the heart is unable to pump with enough force to fight the pull of gravity causing fainting or dizziness. This can often cause fear or panic in patients, meaning nurses and physiotherapists need to be mindful when attempting to mobilise a patient. Often, this is referred to as postural hypertension. To eliminate the fear of fainting or dizziness, the nurse/physiotherapist can utilise the hospital bed frame into a cardiac chair. It is recommended that this bed position is done numerous times throughout the day to acclimatise the patient in a Fowler’s position in preparation for the patients assisted stand.
The heart like any other muscles needs to remain active to stay healthy. Like all muscles in our body, if we do not use them, they start to deteriorate. Myocardial thinning caused by the atrophy limits the effectiveness of the heart as a pump2, and Starlings principle stated following a long period of bedrest there is a marked reduction in blood volume and a weakened venous return. To offset this, we will see an increase in the patients’ heart rate. Corcoran, (1991)3 confirms after four weeks of bedrest the resting heart rate is increased by 10bpm and 40bpm during exercise it can take a patient up to 10 weeks to gain normal exercise tolerance once they become mobile.
Click the links below to read the rest of this series:
How do I Prevent the Complications of Immobility?
Part 4: Gastrointestinal and Renal
Part 5: Musculoskeletal and Bones