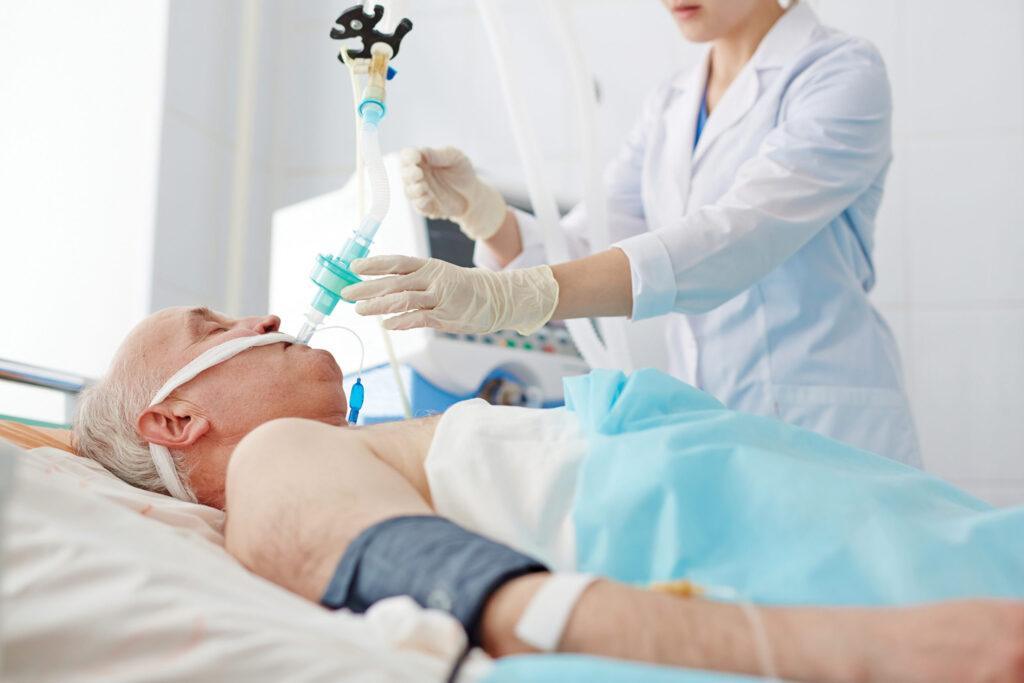
Part 3: How Can I Prevent Complications From Immobility? Haematological
Part 3: Haematological
The excessive production of urine associated with bed rest causes a gradual reduction in plasma volume. After a week 10% plasma volume is lost and around 15% by 4 weeks.1 In early stages of bed rest, the red cell mass remains relatively constant as plasma volume decreases leading to significant increase in blood viscosity. This, along with the decrease in lung function gives an increase in carbon dioxide, and because of these changes to the blood gases it can have serious effects on other vital organs1.
Muscle atrophy caused by reduced mobility affects the red blood cell production, thus reducing the amount of oxygenated blood traveling through the veins. When the patient is bed bound, blood flows to the thoracic veins and right atrium. Cardiac output temporarily increases, and the kidneys may believe that there is too much intravascular volume. The kidneys decrease the release of anti-diuretic hormone (ADH) and “extra” sodium and water are excreted. As a result, the effective circulating blood volume decreases and blood viscosity increases.
Within less than 24 hours of bed rest, increased urine output can cause a gradual reduction in plasma volume which ultimately increases blood viscosity making the blood more susceptible to clot2. Muscle atrophy caused by reduce mobility affects the red blood cell production, thus reducing the amount of oxygenated blood traveling through the veins. The excessive production of urine associated with bed rest causes gradual reduction in plasma volume. After a week 10% plasma volume is lost and around 15% by four weeks.
Virchow’s Triad refers to three factors which when present together dramatically increase risk of DVT forming venous stasis, hypercoagulability and blood vessel damage. Prolonged bed rest activates all three and it has been estimated that up to 13% patients in bed for long periods may develop a DVT.
Venous stasis occurs as the skeletal muscle pump becomes less efficient, and blood flow within the veins in the lower limbs can become slow-moving or stop completely, leading to pooling and venous stasis. Muscle disuse can contribute to thrombus formation in the intramuscular veins. Studies have shown that the intramuscular veins, particularly those in the soleus muscle of the calf, are responsible for 90% of DVT cases that cause a PE in patients confined to bed3. Foot and ankle exercises encouraged by multidisciplinary teams along with anti-embolic stockings widely used in the hospital setting can help to promote venous return.
Hypercoagulability may also occur because blood is pooling, and clotting factors are not cleared by the liver as quickly, meaning the blood is more viscous due to reduced blood plasma but stable levels of red blood cells, all increasing the likelihood of clot formation or thrombosis. Blood vessel damage may also occur due to the inner endothelial lining of arteries is only one cell thick and is extremely delicate.
A deep vein thrombus (DVT) in the thigh veins mean there may be symptoms of venous insufficiency in the distal leg, with redness and pain. Conversely, a deep vein thrombus in the calf veins is more likely to be due to venous stasis. It may extend proximally in the direction of the venous return, with no sign of venous insufficiency, and the patient may even be asymptomatic. The danger of a thrombus in the distal calf veins is that there is an increased risk of the thrombus embolising via the inferior vena cava (toward the right side of the heart and the pulmonary vasculature) and creating a pulmonary embolus.5
Blood clots or emboli may travel to any part of the body but are common in three major areas:
- Pulmonary – where they block the blood flow in the lungs.
- Cerebral – potentially blocking the circulation in the brain causing a stroke
- Coronary – thus blocking the circulation in the heart causing the patient to have a myocardial infarction.
Read part 4 where we discuss the effects of immobility on the gastrointestinal and renal systems.
Click the links below to read the rest of this series:
How do I Prevent the Complications of Immobility?
Part 5: Musculoskeletal & Bones