Part 1: The Science of Surfaces Series
Part 1: How do Pressure Ulcers Form?
Overview
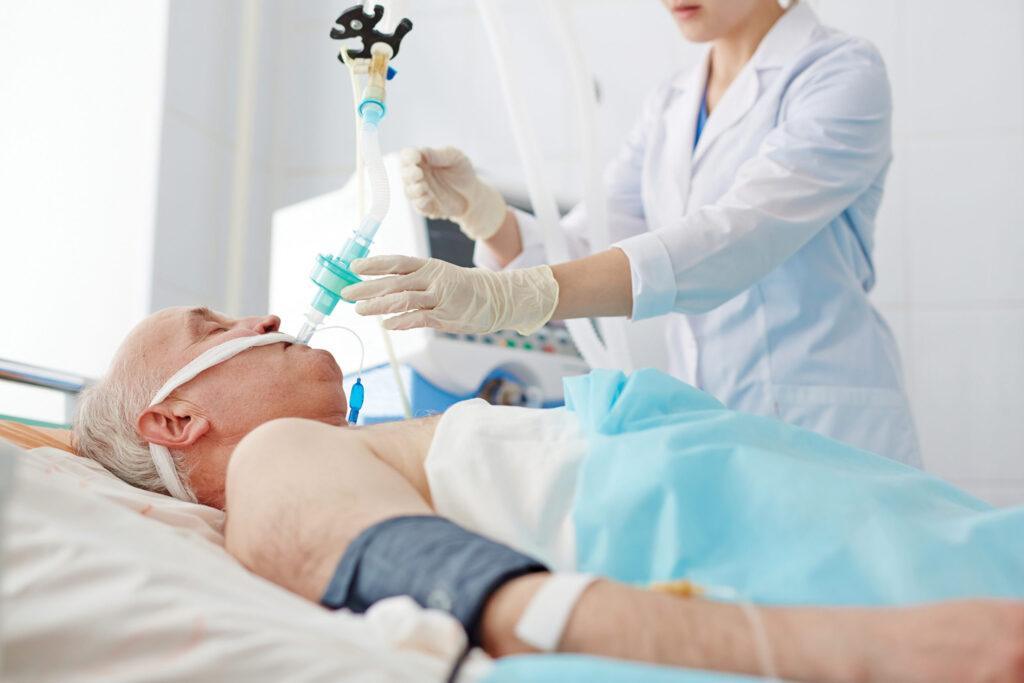
Pressure ulcers (also known as pressure sores, bed sores, wounds, or pressure injury) are damage to the skin and the underlying tissues, primarily caused by prolonged pressure1. Pressure ulcers can occur in several ways but are often deemed as preventable2.
NHS Inform 20203 deem pressure ulcers to be damage that breaks down the skin and the underlying tissues, due to an area of skin being placed under pressure. This can occur due to lots of pressure being applied over a short period of time or pressure being applied over a long period of time3. This added pressure disturbs the normal blood flow around the skin and without this supply, the skin becomes starved of oxygen and nutrients and starts to breakdown, damaging the tissues leading to a pressure ulcer3.
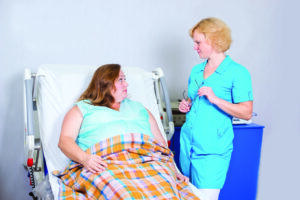
All patients are potentially at risk of developing pressure ulcers; however, they are more likely to develop in individuals who are seriously sick, have impaired nutrition, impaired mobility, have a neurological condition, deformity, or poor posture2.
The skin is the largest organ of the body, holding the content of the body together consisting of two layers; the epidermis and the dermis4. The epidermis is the outer layer, and the dermis is the inner layer which forms elastic beds of connective tissue, providing strength and support4.
The skin has a multitude of functions such as protection from general wear and tear, infection, chemicals and receiving stimuli from the outside to name but a few functions4. The epidermis is the outer layer of the skin and its prime function is to act as a physical and biological barrier to the external environment. This is made up of four layers (sometimes five with the thickest skin), and it prevents penetration by allergens or irritants5. The dermis forms the inner layer of the skin and its functions include protection, cushioning the deeper structures from mechanical injury, provide nourishment to the epidermis and wound healing with the primary role of sustaining and supporting the epidermis5.
The skin is a versatile organ that can be exposed to various trauma6. A serious occurrence of trauma could lead to the loss of the skin integrity which is the barrier to protect against infection, and lead to the formation of pressure ulcers6. Pressure ulcers can range from minimal discolouration to the skin to potentially life-threatening skin damage affecting all layers from the epidermis, dermis to the muscles and sometimes even to the bone6.
There are four main factors that contribute to the formation of pressures ulcers: pressure, shear, friction, and moisture or a combination of these7. In more recent years, it has also been identified that medical devices are also an influencing factor on pressure ulcer formation. Within this series, we will be taking a look into each one of these contributing factors in further detail.
Click here for part 2 where we look at pressure.
The links to the other parts of this series are below: