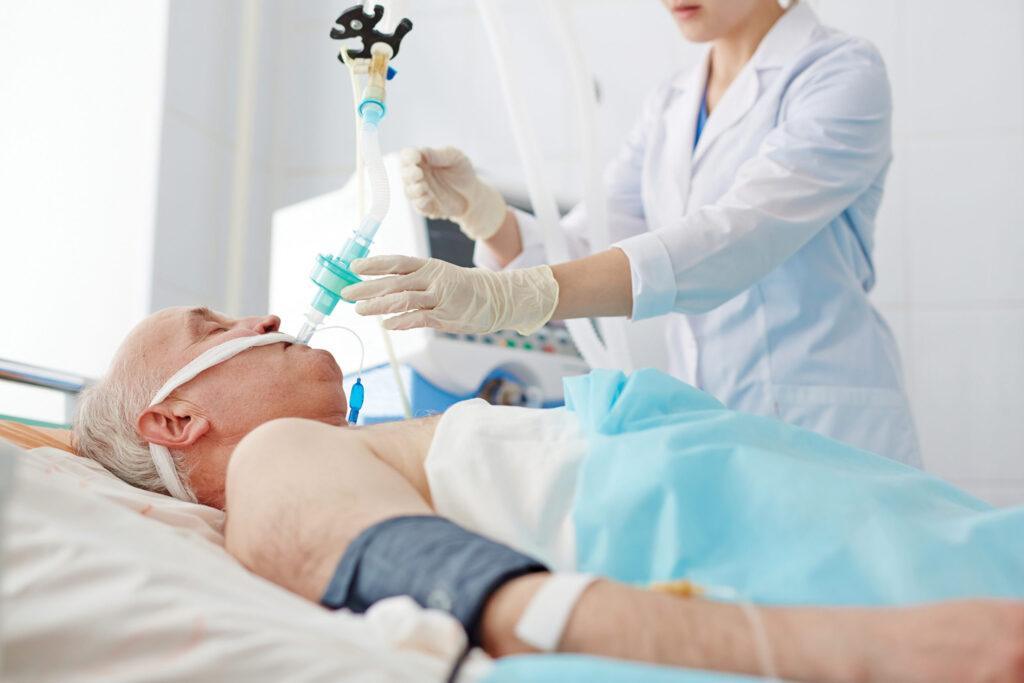
Rehabilitating Long Covid Patients Effectively
It has been estimated that two million people in the UK are living with Long Covid and 66% report symptoms are adversely affecting day-to-day activities. It’s also been addressed that “safe and effective rehabilitation is increasingly recognised as a fundamental health service that people living with Long Covid have the right to access1”
What is ‘Long Covid’? The NHS2 state: “For some people, coronavirus (COVID-19) can cause symptoms that last weeks or months after the infection has gone. This is sometimes called post-COVID-19 syndrome or “Long Covid”.
Paul Chrisp, Director of the Centre for Guidelines at NICE also states: “Recovery from any infectious illness can take time and although most people with COVID-19 will recover completely within a few weeks from the onset of symptoms, we know that a sizeable minority will continue to have symptoms for 12 weeks or more afterwards, regardless of how ill they were initially or whether they were hospitalised.3”
Immobility and Long Covid: Based on real-time assessment of community transmission findings (REACT2)4, it was noted symptoms of those diagnosed with Long Covid included:
- Small cluster with respiratory symptoms
- Larger cluster where tiredness was the dominant symptom
- Participants noted symptoms had a “significant effect on my daily life”
It is reasonable to suggest that those who are breathless and fatigued may become less mobile. Immobility is most associated with muscle deconditioning but effects all of the body systems creating problems such as5:
- Cardiac – postural hypertension/cardiac deconditioning
- Respiratory – respiratory tract infections
- Haematological – DVTs
- Gastrointestinal – constipation
- Renal – urinary retention and UTI
- Musculoskeletal – muscle atrophy, contractures, reduction in bone density and pressure damage to skin
- Psychological – confusion, depression and loss of confidence
Other impacts of immobility associated with respiratory infections (such as Covid-19) include:
- Study of those surviving ARDS show persistent functional disability one year post-discharge, and exercise limitation five years post-admission6
- It is widely recognised that early activation directly influences the long-term rehabilitation outcomes for patients who have been in an immobilised state in acute care
- Over the pandemic, it has become apparent that the Covid-19 virus adds another level of complexity to this already demanding set of physical and physiological circumstances
As such, the importance of early active rehabilitation of the patient in order to enhance long term recovery and quality of life is paramount.
What can we do to minimise the effects of immobility? Dr Colin Robertson who presented at Medstrom’s Long Covid webinar, suggested to minimise the effects of immobility, three steps should be taken:
- Early activation – no movement is too small
- Alter posture — prone, supine, side-lying, seated, near upright
- Adopt a schedule — regular and often
Medstrom Aria 6000 and MMO 6000:
Launched in 2021 to he
This superior coupling of products enables a patient to be put in a full-egress position via the touch of a button, allowing patients to effortlessly progress from a sitting to a standing position safely and easily. It fundamentally helps to:
- Empower patient independence
- Support early mobilisation safely
- Prevent pressure ulcers
References:
- Ref: Chartered Society of Physiotherapy. CSP updates Covid-19 community rehab standards. [online] https://www.csp.org.uk/news/2021-07-14-csp-updates-covid-19-community-rehab-standards
- https://www.nhs.uk/conditions/coronavirus-covid-19/long-term-effects-of-coronavirus-long-covid/
- https://www.nice.org.uk/news/article/nice-sign-and-rcgp-set-out-further-details-about-the-uk-guideline-on-management-of-the-long-term-effects-of-covid-19)
- https://www.imperial.ac.uk/medicine/research-and-impact/groups/react-study/studies/react-long-covid/
- https://www.nursingtimes.net/clinical-archive/cardiovascular/effects-of-bedrest-1-introduction-and-the-cardiovascular-system/7026883.article
- Herridge et al. 2003. One-Year Outcomes in Survivors of the Acute Respiratory Distress Syndrome. N Engl J Med 2003; 348:683-693