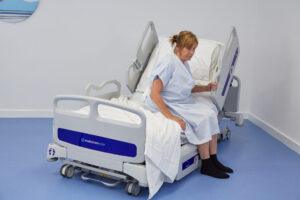
Role of the Hospital Chair in Patient Recovery
The right hospital chair, used at the right time, can help to improve clinical outcomes. This is particularly true for older patients at risk of rapid deconditioning. In this article, we look at the challenges elderly patients can face, and the benefits they can gain from sitting out of bed, getting dressed, and moving.
Challenges of Hospitalisation for Older People
Immobility can quickly lead to deconditioning, which increases frailty, which in turn reduces mobility further. This can happen quickly in an older hospital patient confined to bed:

There is lots of published evidence which clearly demonstrates this problem, including:
- Up to 65% of older hospital patients experience a decline in their ability to walk.1
- During acute hospitalisation, patients spend up to 95% of their time in bed, and on average just 12% in a hospital chair.2,3
- Reduced tissue oxygenation increases pressure ulcer risk.4
- Deconditioning starts from day 2 of hospitalisation, with up to 20% of muscle mass lost in the first week of bedrest.5
- In patients aged 80 or over, 10 days of being bedbound and inactive can equate to 10 years of muscle wastage.6
- Lack of a suitable chair and/or mobilisation aid keeps patients in bed, resulting in both physical and cognitive complications.7
Early Mobilisation Matters
Early mobilisation is known to reduce complications of immobility and deconditioning. Two successful NHS campaigns have raised awareness about deconditioning and the benefits of getting out of bed, getting dressed, and mobilising early; ‘Sit Up, Get Dressed, Keep Moving’, and ‘End PJ Paralysis’.8 In addition, clinical trials have consistently shown a reduced length of hospital stay in patient groups who mobilised early.9-14
For elderly patients, there can be a difficult balance to strike between time spent in bed versus up in a chair. Sitting out of bed gives both physical and psychological benefits,15 but patients at risk of pressure damage could be at increased risk. This is due to higher pressures because the patient’s upper body weight is concentrated in a small area.16, 17
Choosing the Right Hospital Chair
The correct choice of hospital chair is essential to maximise benefits for the patient. It must offer the correct level of support, and be the right size. For example, the wrong seat height increases the risk of falls,18 and the wrong depth, width or height can increase pressure ulcer risk.19 It’s also very important to assess whether a pressure care cushion is needed to provide extra support for at risk patients.
Other Articles in the ‘Commit to Sit’ Series
Part 2: Patient chairs – types and selection.
Part 3: Adding a pressure care cushion to a chair.
References
-
Kortebein P, Symons TB, Ferrando A, et al. Functional impact of 10 days of bed rest in healthy older adults. J Gerontol A Biol Sci Med Sci. 2008;63(10):1076-1081.
-
Arora A. Prevalence, severity, and nature of preventable patient harm across medical care settings: systematic review and meta-analysis. BMJ2019;366:l4185.
-
Falvey JR, Mangione KK, Stevens-Lapsley JE. Rethinking Hospital-Associated Deconditioning: Proposed Paradigm Shift. Phys Ther. 2015;95(9):1307-1315.
-
What are the risk factors for pressure ulcers? NICE Clinical Knowledge Summaries (2024). Available at: Risk factors | Background information | Pressure ulcers | CKS | NICE
-
Laidler D. Physiological results relating to inactivity (2021). NHS Education for Scotland. Available at: https://learn.nes.nhs.scot/49141/rrheal/nhs-highland-virtual-lectures/physiological-results-relating-to-inactivity
-
2019 Adult InpatientSurvey. Statistical release. CQC. Available online: pdf (cqc.org.uk)
-
Chen Y et al (2022) Hospital associated deconditioning: Not only physical, but also cognitive. Int J Geriatr Psychiatry 37(3):10.1002.
-
Arora A. Recondition the nation. NHS (2023). Available at: NHS England » Recondition the nation
-
Bergbower EAS et al. A novel early mobility bundle improves length of stay and rates of readmission among hospitalized general medicine patients. J Community Hosp Intern Med Perspect. 2020;10(5):419-425.
-
Mundy LM et al. Early mobilization of patients hospitalized with community-acquired pneumonia. Chest. 2003;124(3):883–889.
-
Munin MC et al. Early inpatient rehabilitation after elective hip and knee arthroplasty. JAMA. 1998;279(11):847–852.
-
Hoyer EH et al. Promoting mobility and reducing length of stay in hospitalized general medicine patients: A quality-improvement project. J Hosp Med. 2016;11(5):341–347.
-
Larsen T et al. Effect of early mobility as a physiotherapy treatment for pneumonia: a systematic review and meta-analysis. Physiother Can. 2019;71(1):82–89.
-
Hartley PJ et al. Earlier Physical Therapy Input Is Associated With a Reduced Length of Hospital Stay and Reduced Care Needs on Discharge in Frail Older Inpatients: An Observational Study. J Geriatr Phys Ther. 2019;42(2):E7-E14.
-
Stoneley, S. Sit Out, Get Out (S.O.G.O) — #EM3: East Midlands Emergency Medicine Educational Media (2016). Available at: Sit Out, Get Out (S.O.G.O) — EM3
-
Orsted, HL et al. International review. Pressure ulcer prevention: pressure, shear, friction and microclimate in context. A consensus document (2010). London. Wounds International.
-
Krouskop TA. A synthesis of the factors that contribute to pressure sore formation. Med Hypothesis (1983).11(2):255-67.
-
Martindale D (2021). Calculating bed height for hospital patients using popliteal measurement. Nursing Times [online]; 117: 10.
-
Stephens M and Bartley CA (2018) Understanding the association between pressure ulcers and sitting in adults what does it mean for me and my carers? Seating guidelines for people, carers and health & social care professionals. J Tissue Viability 27: 59-73.